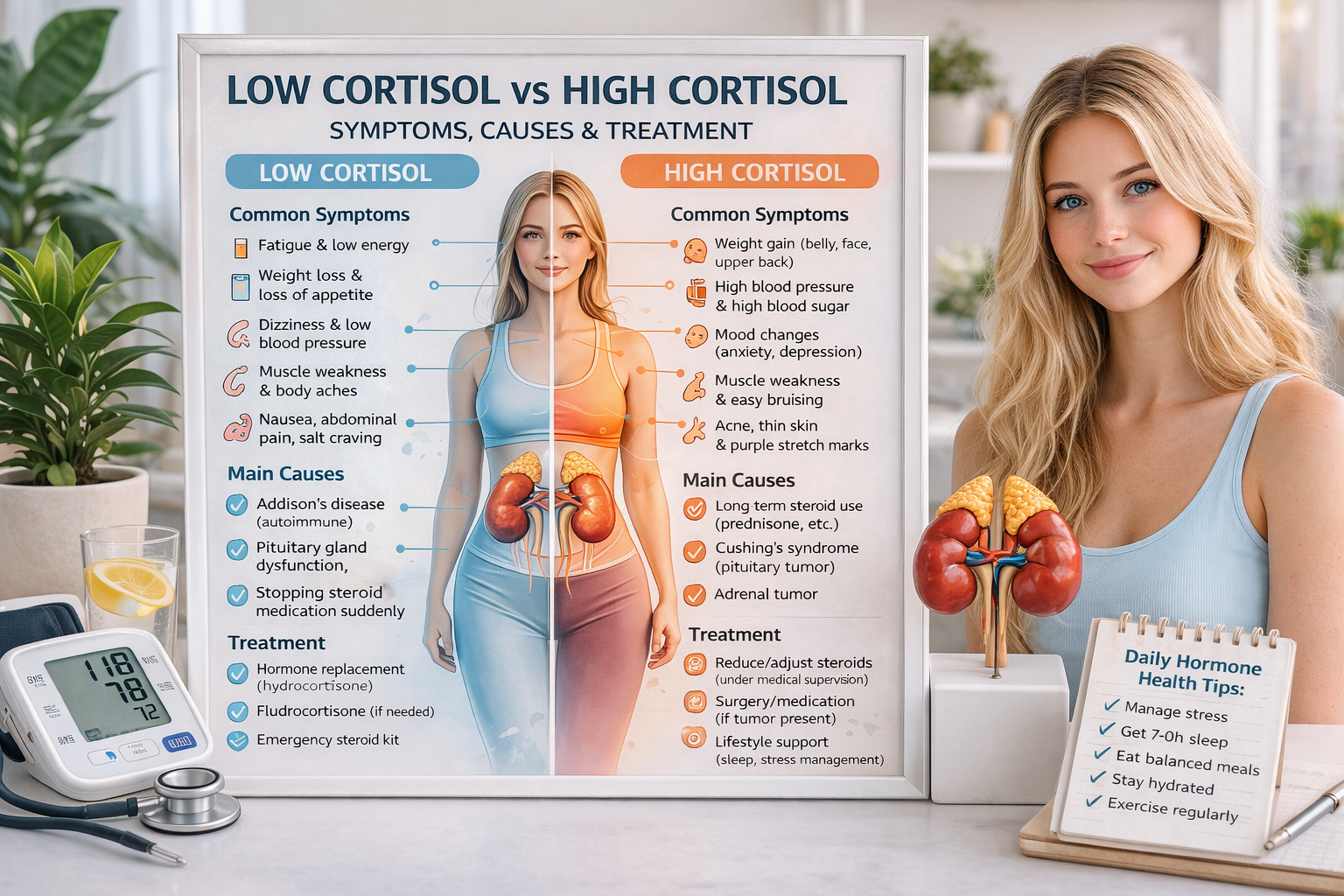
Low cortisol vs high cortisol is an important comparison because cortisol is often called the body’s “stress hormone,” but its role goes far beyond stress. It helps regulate blood pressure, blood sugar, inflammation, metabolism, and your response to illness. When cortisol is too low or too high for too long, the body can start sending warning signs that should not be ignored. Low cortisol is usually linked to adrenal insufficiency, while high cortisol over time may be caused by steroid medicines or a condition such as Cushing’s syndrome. The tricky part is that symptoms can look like common issues such as fatigue, weight changes, anxiety, or poor sleep, which is why proper testing matters.
Table of Contents
Low Cortisol vs High Cortisol: Symptoms Compared
When cortisol is too low, the body may struggle to maintain energy, blood pressure, and a normal stress response. Common symptoms include fatigue, muscle weakness, loss of appetite, weight loss, abdominal pain, dizziness, nausea, and salt craving. In severe cases, adrenal crisis can happen, which is a medical emergency.
When cortisol is too high for a long period, the body may start showing signs such as weight gain around the midsection and upper back, high blood pressure, high blood sugar, muscle weakness, easy bruising, mood changes, acne, poor sleep, and thinning skin. In women, excess hair growth and irregular periods can also happen.
A key point here is that “high cortisol” in medical care does not simply mean feeling stressed. Everyday stress can affect cortisol levels temporarily, but true cortisol excess, such as Cushing’s syndrome, needs medical testing and a cause-based diagnosis.

Causes of Low Cortisol
Low cortisol most often happens because the adrenal glands cannot make enough hormones, or because the brain is not sending the right signals to the adrenal glands.
The main causes include:
1. Primary adrenal insufficiency
This is when the adrenal glands themselves are damaged. Addison’s disease is a well-known form, and autoimmune disease is a leading cause. (MedlinePlus)
2. Secondary adrenal insufficiency
This happens when the pituitary gland does not make enough ACTH, the hormone that tells the adrenal glands to produce cortisol. Pituitary tumors, injury, infection, or surgery can contribute.
3. Tertiary adrenal insufficiency
A common cause is suddenly stopping corticosteroid medicine after using it for a long time. The body may need time to restart normal cortisol production.
Causes of High Cortisol
High cortisol usually comes from one of two paths: medication-related cortisol excess or the body producing too much cortisol on its own.
1. Long-term corticosteroid use
This is the most common cause of Cushing’s syndrome. Medicines such as prednisone, dexamethasone, and similar glucocorticoids can raise cortisol levels in the body when used in high doses or for long periods.
2. Pituitary tumors
Some pituitary tumors produce too much ACTH, which pushes the adrenal glands to make excess cortisol. This form is called Cushing’s disease.
3. Adrenal tumors or ectopic tumors
An adrenal tumor may directly produce extra cortisol. Some tumors outside the pituitary, often in the lungs or elsewhere, can also produce ACTH and drive cortisol too high.
Solutions and Treatment
How is low cortisol treated?
Low cortisol is usually treated with hormone replacement, most often hydrocortisone. Some people also need fludrocortisone if aldosterone is low. During illness, injury, or surgery, doses often need to be increased because the body needs more cortisol under physical stress.
People with diagnosed adrenal insufficiency may also be taught how to use an emergency hydrocortisone injection in case of adrenal crisis. (MedlinePlus)
How is high cortisol treated?
Treatment depends on the cause. If steroid medicine is the reason, the dose is usually reduced gradually under medical supervision, not stopped suddenly. If the cause is a tumor, treatment may include surgery, medicine, radiation, or other targeted care.
Lifestyle support
Healthy sleep, regular movement, stress management, and balanced meals can support overall hormone health, but they do not replace diagnosis or treatment when true cortisol disorders are present. Symptoms of cortisol imbalance should be medically evaluated, especially if they are persistent or severe.
When to See a Doctor
See a healthcare professional if you have ongoing fatigue, unexplained weight loss or gain, dizziness, muscle weakness, easy bruising, abnormal blood pressure, or symptoms that keep getting worse. Seek urgent care if low cortisol is suspected and severe vomiting, confusion, collapse, or signs of adrenal crisis appear.
FAQ
Can stress alone cause high cortisol?
Stress can temporarily increase cortisol levels, but that is not the same as diagnosed Cushing’s syndrome. Persistent symptoms need medical evaluation.
Is low cortisol dangerous?
Yes. Untreated adrenal insufficiency can lead to adrenal crisis, which is an emergency.
How do doctors test cortisol levels?
Cortisol can be checked through blood, urine, or saliva testing. Doctors may order more than one type of test depending on the situation.
References
- NIDDK: Adrenal Insufficiency & Addison’s Disease (NIDDK)
- NIDDK: Cushing’s Syndrome (NIDDK)
- MedlinePlus: Cortisol Test (MedlinePlus)
- MedlinePlus: Addison Disease / Cushing Syndrome (MedlinePlus)
